However, the complications of low intraocular pressure (IOP) and silicon oil (SO) dependence after retinectomy are not friendly for the long-term prognosis of patients. There have been a few reports on the treatment of Re-RD after vitrectomy for RRD, and the surgical methods are relatively radical, retinectomy for all, combined with scleral buckling for all, or retinectomy combined with scleral buckling. However, this treatment remains challenging. Re-RD after vitrectomy with gas tamponade or vitrectomy with silicone oil removal (vitrectomy) progresses rapidly and may easily lead to proliferative vitreoretinopathy (PVR). 
Although such research can provide a certain understanding of the overall situation and prognosis of Re-RD, it is not of great clinical significance or reference value for a certain group of people. 
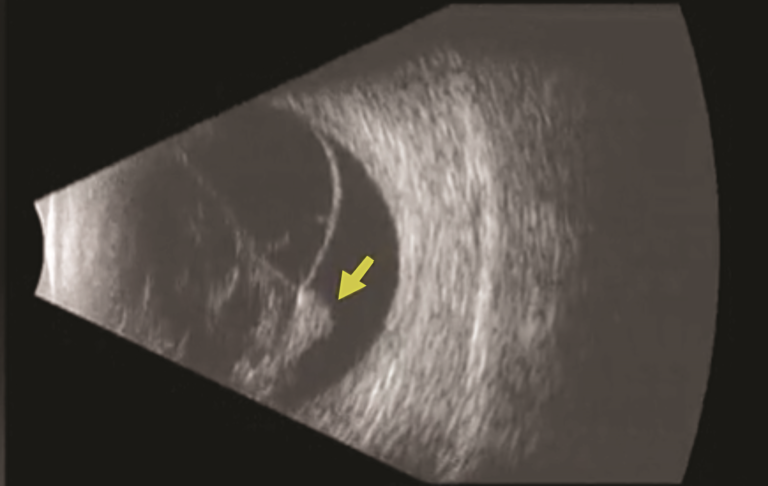
(3) Even though some studies evaluated the effectiveness of reoperation for Re-RD patients according to the initial surgical method respectively, the vitreous status of Re-RD patients after vitrectomy was different, including both silicone oil filled or no tamponade eyes. (2) Although some authors uniformly included patients who had Re-RD after surgery for RRD, the primary surgical methods in the same study were different, including scleral buckling, vitrectomy, or retinopexy. (1) In many articles, patients with various etiologies, such as RRD, vascular diseases, or penetrating injury, were included in the analysis of the characteristics of Re-RD. Previous clinical studies on Re-RD had the several disadvantages. Reports on the treatment and prognosis of Re-RD are relatively fewer than those of RRD in the past. Recurrent retinal detachment (Re-RD) is one of the most common reasons affecting the prognosis of surgery for rhegmatogenous retinal detachment (RRD). In Re-RD patients with no definite retinal break detected preoperatively, the retinal hole usually shows small crevice-like changes alongside a large number of original laser pigment scars. Revitrectomy without retinectomy or scleral buckling can effectively treat Re-RD in post-vitrectomy eyes. In the contralateral eyes, 15% already had vision-damaging disease, and the incidence of eyesight-threating lesions was 5.9% during follow-up. The single-operation complete retinal reattachment rate was 75%, the complete retinal reattachment rate was 80%, and the final incomplete retinal reattachment rate was 90%. Among the 12 eyes with no break detected before surgery, 11 (92%) were found to have a small crevice-like break beside the pigment scar of a large number of original laser spots. The final BCVA was negatively correlated with the axial length and positively correlated with the preoperative BCVA. Patients with phakic eyes, those undergoing only one surgery, and those with more than one break had better final BCVA. This is a retrospective case series analyzed the ocular characteristics of 20 recurrent and contralateral eyes, evaluated the significance of the associations between variables before reoperation and the final best-corrected visual acuity (BCVA), and calculated the outcome of revitrectomy. This study aimed to analyze the clinical characteristics of Re-RD in post-vitrectomy eyes with RRD and surgical outcomes after revitrectomy without combining it with retinectomy or scleral buckling. Previous clinical studies of Re-RD were not specific. Recurrent retinal detachment (Re-RD) usually affects the prognosis of surgery for rhegmatogenous retinal detachment (RRD). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
